
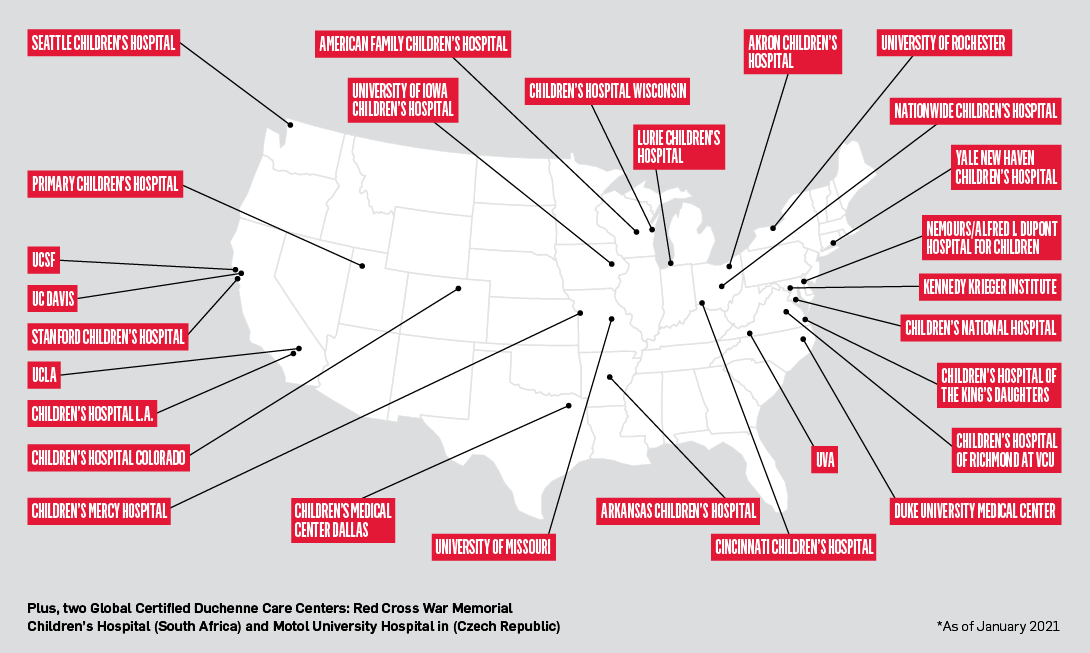
PPMD’s Certified Duchenne Care Center (CDCC) Program was developed to make comprehensive Duchenne care and services, provided in agreement with the CDC Care Considerations, available and accessible to as many families as possible, and to strengthen clinical trial results by decreasing variability in care among clinical trial subjects. Since the first certification in 2014, the CDCC network has grown to 28 centers across the United States, includes more than 500 medical providers, and serves more than 3,600 patients and their families.

2020 CDCC Updates
PPMD was thrilled to kick the year off by hosting the third Duchenne Healthcare Professionals Summit, which was held January 22-24, 2020. Through this collaborative meeting, attendees from over 40 academic institutions – including 23 CDCCs, 4 international providers, and 14 additional US institutions providing pediatric and adult Duchenne care – dove into topics including lessons learned from clinical trials, the first FDA approvals for drugs treating Duchenne, exploration of uses for patient data to advance clinical care and research, and much more.
While the 2021 Summit was cancelled due the effects of the pandemic, we look forward to regathering in January 2022 in Reno, Nevada, for the next Duchenne Healthcare Professionals Summit.
New Certifications in 2020
Despite a sudden halt to in-person travel due to the COVID-19 global pandemic, the Certified Duchenne Care Center Program forged ahead announcing certifications of two new centers. In the spring, Kennedy Krieger Institute became the first center in the CDCC network to achieve dual certification status, demonstrating excellence delivering both pediatric and adult Duchenne care.
The CDCC program also grew to include Akron Children’s Hospital, serving patients in northeast Ohio and the Ohio Valley, and Children’s Health and UT Southwestern Medical Center, the first certification in the state of Texas. With the addition of Akron Children’s and UT Southwestern, the CDCC network now includes 28 centers, one of which is an adult certified center and another dually-certified. We look forward to continuing to grow the CDCC network in 2021 and beyond with the goal of bringing certified Duchenne care to every market in the United States to ensure that everyone living with Duchenne has access to excellent, standardized care regardless of where they live.
Thriving in a virtual world
While the COVID-19 pandemic led to a sudden halt to travel, community engagement opportunities, and in-person clinic visits, the CDCCs rose to the challenge. Centers quickly pivoted to implement multi-disciplinary telemedicine visits to ensure the safety and health of those living with Duchenne. Additionally, CDCC member centers lent their expertise in the creation of a COVID-19 Information Center, housed on the PPMD website, to offer accurate, concise information about the pandemic for families to easily access. A series of webinars with speakers from throughout the CDCC network offered opportunities to discuss emerging topics and tips and tricks for safely navigating Duchenne care in the midst of crisis.
Also announced in 2020 was the first-ever Certified Duchenne Care Center Inter-Institutional Collaborative Grant program, which fosters collaboration across CDCCs despite our virtual world, encouraging centers to partner together in collaborative care improvement projects. Awards of up to $150,000 will be announced in late Q3 2021 and will address three areas of care: diagnosis and early intervention, transitional or adult care, and general pediatric care.
2020 ANNUAL REPORT FOR CDCC MEMBER CENTERS
The table below describes the 2020 annual report for each center.
| Center | Date of Certification | Certification Type | Director(s) | Coordinator | # Duchenne/ Becker Patients | In Good Standing | Notes |
|---|---|---|---|---|---|---|---|
| Akron Children's Hospital | 6/16/2020 | Pediatric | Katherine Mosher (PM&R) | Noelle Buso, MSW | 50 | yes | New certification in 2020 |
| American Family Children's Hospital | 9/1/2018 | Pediatric | Jennifer Kwon (neurology) | Cory Sieburg APNP | 30 | yes | Departure of Laura Banning, addition of Kylie McGinn to clinic coordination staff |
| Ann and Robert H. Lurie Children's Hospital | 12/1/2016 | Pediatric | Nancy Kuntz | Kristen Alianello | 141 | Yes | Currently recruiting new pulmonologist |
| Arkansas Children's Hospital | 10/1/2019 | Pediatric | Aravindhan Veerapandiyan | Tiffany Boyd RN | 100 | yes | none to report |
| Children's Hospital Colorado | 6/2014 (6/2019) | Pediatric | Sue Apkon (PM&R), Julie Parsons (neurology) | Alison Ballard CNPN | 180 | yes | Established significant telehealth capabilities |
| Children's Hospital of the King's Daughters | 1/29/2019 | Pediatric | Crystal Proud (neurology) | Erika Paradiso RN and Tanicia Johnson | 73 | yes | none to report |
| Children's Hospital Los Angeles | 3/1/2016 | Pediatric | Leigh Ramos-Platt | Arlene Deseo RN | 179 | yes | none to report |
| Children's Hospital of Richmond VCU | 8/1/2019 | Pediatric | Amy Harper | Suzanne Spivey; Nicole Olive, MSN, RN | 70 | yes | New nurse navigator, Nicole Olive; several patients trasitioned successfully to adult clinic |
| Children's Hospital Wisconsin | 11/6/2018 | Pediatric | Matthew Harmelink (neurology) | Gretchen Heckel MSN | 45 | yes | none to report |
| Children's Medical Center Dallas/UTSW | 4/29/2020 | Pediatric | Diana Castro (neurology), Susan Iannaccone (neurology) | Connie Choudhury | 200 | yes | New certification in 2020 |
| Children's Mercy Hospital | 3/1/2016 | Pediatric | Ann Modrcin (PM&R) | Alexis Hazlett | 85 | yes | none to report |
| Children's National Hospital | 11/1/2014 | Pediatric | Diana Bharucha Goebel (Neurology) | Kathleen Smart | 52 | yes | Newly implemented access to multi-disciplinary telmedicine capabilities |
| Cincinnati Children's Hospital Medical Center | 6/2014 (6/2019) | Pediatric | Cuixia Tian (neurology), Mary McMahon (PM&R) | Allison Egbert, Wendy Chouteau | 418 | yes | Addition of Neepa Gurbanami, Carolyn Burrows, Krista Nee, Danielle Graef |
| Duke Children's Neuromuscular Center | 6/1/2015 | Pediatric | Edward Smith (neurology) | Pam Green, RN | 188 | yes | recertified 6/2020; departureof Pam Green, RN |
| Kennedy Krieger Institute | 11/2014 (11/2019)/ 4/1/2020 (Adult) | Dual | Jessica Nance (neurology) and Doris Leung (neurology) | Angie Lasseth, Michael Munchel | 250 | yes | Departure of Dr. Kathryn Wagner; dual certification status |
| Lucile Packard Children's Hospital Stanford | 3/1/2015 | Pediatric | John Day (neurology) | Jessica Guzman | 133 | yes | Recertified 9/2020 |
| Nationwide Children's Hospital | 4/2014 (4/2019) | Pediatric | Kevin Flanigan (neurology) | Cassandra Karingada NP Rita Peirano RN | 435 | yes | none to report |
| Nemours AI Dupont | 8/1/2017 | Pediatric | Mena Scavina (neurology) | Jennifer Hultberg | 56 | yes | New physical therapist, new social worker, new orthopedist, new dietician |
| Seattle Children's | 9/2014 (9/2019) | Pediatric | Seth Perlman (Neurology) | vacant | 85 | yes | none to report |
| UC Davis | 1/1/2017 | Pediatric | Craig McDonald (PM&R), Nanette Joyce (PM&R) | Erica Goude, Gina Fortugno | 327 | yes | A number of changes to staff |
| UCLA | 3/1/2016 | Pediatric | Stan Nelson, Perry Sheih, Nancy Halnon | Jenna Gewirtz | 130 | yes | Addition of Dr. Payam Soltanzadeh to young adult clinic, new research RN, new pediatric geneticist, new social worker |
| UCSF Benioff Children's Hospital | 11/1/2017 | Pediatric | Jonathan Strober (neurology) | Audrey Glancy | 44 | yes | Addition of Dr. Alexander Fay (neurology), new CGC, RD, OT |
| University of Iowa | 2/1/2015 | Pediatric | Kathy Mathews (neurology) | Christina Trout RN, MSN | 115 | yes | Recertified 8/2020 |
| University of Missouri | 9/1/2019 | Adult | Raghav Govindarajan (neurology), Vovanti Jones (PM&R) | Amanda Hueffmeier, Natalie Taylor | 22 | yes | none to report |
| University of Rochester | 2/11/2019 | Pediatric | Emma Ciafaloni (neurology) | Erin Collins | 120 | yes | none to report |
| University of Utah/Primary Children's Hospital | 4/26/2019 | Pediatric | Russell Butterfield (neurology) | Meagan Bernatz APRN | 105 | yes | none to report |
| University of Virginia Children's Hospital | 11/28/2018 | Pediatric | Rebecca Scharf (neurodevelopmental pediatrics and neurology) | Lorie Nouwairi RN, Chelsea Masterson | 48 | yes | none to report |
| Yale New Haven Children's Hospital | 12/1/2016 | Pediatric | Cristian Ionita (neurology) | Louise Lanouette | 50 | yes | none to report |
THE MONITORING PROCESS
The CDCC program is monitored by the CDCC Certification Committee, which consists of 19 individuals who represent several areas of neuromuscular subspecialty care, parents, adults living with Duchenne, and industry partners, and operates under the guidance of PPMD’s Vice President of Clinical Care and Education. This committee reviews each application and site visit summary, and makes recommendations and requirements regarding each center’s potential certification. If center issues arise, this committee convenes to discuss the issue and potential solutions, and discusses these solutions with the center. It is then the responsibility of the committee to follow up on the resolution to ensure that that recommendations or requirements are followed and that the issue is resolved. By engaging in this rigorous and collaborative process, the committee is able to maintain a high level of expectation of each partner center, ensuring the highest quality of care for people living with Duchenne.
YOUR INPUT IS VITAL
The Clinical Experiences surveys we ask you to complete each year let the CDCC Certification Committee know what elements of care and services you are receiving, and what is going well or could use improvement in the delivery of care and services you receive at your center. We collate all of the responses per center, and at the end of the year provide a single, anonymized report to each center to support a process of continual improvement to ensure that you receive the best care possible. Your voice matters!
Completing the Clinical Experiences Survey annually is vital to the continuous improvement of member centers and the CDCC program at large. Click the link below to complete the survey to ensure your voice is heard.
Complete the Clinical Experiences Survey >PPMD IS DEDICATED TO IMPROVING THE CARE OF EVERY SINGLE PERSON LIVING WITH DUCHENNE
In addition to the expertise offered by the expert clinicians at our CDCCs, PPMD is available to offer medical guidance when needed, referral and connection to appropriate medical personal and genetic counseling to patients, parents, and providers. We are here to support you! To schedule a time with our genetic counselors to discuss your questions about genetics and clinical trials, book an appointment during office hours. For questions about care, reach out to the PPMD care team.
PPMD is extremely proud of what the CDCC Program has been able to accomplish in the last six years, but we have not done it alone. With the help of compassionate and dedicated clinicians and families, we have initiated a program that we hope will work to provide everything that our Duchenne community will need for decades to come.
REMINDERS FOR PARENTS IN EMERGENCY SITUATIONS:
If you are headed to the emergency room or the hospital, please remember:
- Take the PPMD emergency card with you
- Take a copy of the summary of your last neuromuscular visit with you or a brief 1 page summary of your/your child’s care
- Download, and keep handy, thePPMD mobile app
- Take any equipment that you use at home (cough assist, BiPAP, etc.) and medications that you take, with you
- Take a copy of your last ECG with you. (All people living with Duchenne have an abnormal baseline ECG. Providing the emergency team with your baseline heart rate and rhythm will help them to know if anything has changed.)
- Keep the information regarding oxygen use and appropriate anesthesia available for you and the emergency room staff
- Call your neuromuscular team and let them know what is happening
- Be sure that your neuromuscular team is talking with the emergency staff and are guiding your care
- If you/your child has developed an“emergency care plan,” take that as well



 by: Parent Project Muscular Dystrophy
by: Parent Project Muscular Dystrophy


